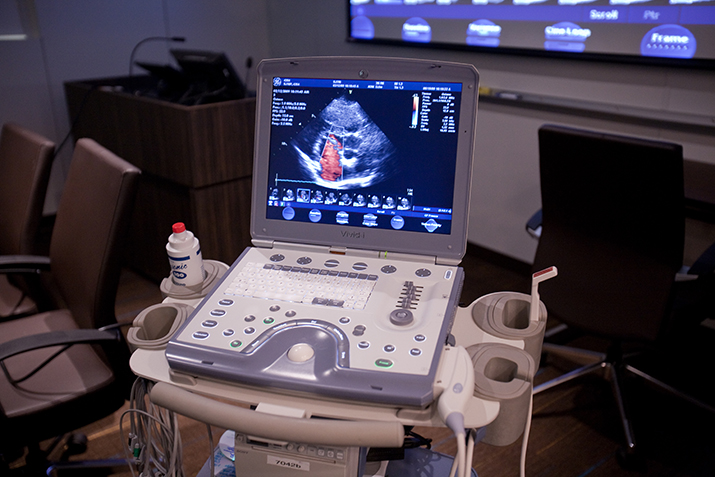
The National Center for Biotechnology Information describes mechanical circulatory assist devices as, “commonly used in the treatment of severe heart failure as bridges to cardiac transplant, as destination therapy for patients who are not transplant candidates, and as bridges to recovery and “decision-making.” These devices, which can be used to support the left or right ventricles or both, restore circulation to the tissues, thereby improving organ function. Left ventricular assist devices (LVADs) are the most common support devices. To care for patients with these devices, health care providers in emergency departments (EDs) and intensive care units (ICUs) need to understand the physiology of the devices, the vocabulary of mechanical support, the types of complications patients may have, diagnostic techniques, and decision-making regarding treatment. Patients with LVADs who come to the ED or are admitted to the ICU usually have nonspecific clinical symptoms, most commonly shortness of breath, hypotension, anemia, chest pain, syncope, hemoptysis, gastrointestinal bleeding, jaundice, fever, oliguria and hematuria, altered mental status, headache, seizure, and back pain. Other patients are seen for cardiac arrest, psychiatric issues, sequelae of non-cardiac surgery, and trauma. Although most patients have LVADs, some may have bi-ventricular support devices or total artificial hearts. Involving a team of cardiac surgeons, perfusion experts, and heart-failure physicians, as well as ED and ICU physicians and nurses, is critical for managing treatment for these patients and for successful outcomes.”
What’s the current state of preclinical work for advancements in circulatory assist devices? GCMI’s Michael Sweet recently shared his insights in the following Q&A with our partner Paul Snyder at Write2Market.
Paul: What’s the current state of circulatory or ventricular assist device technology approved for clinical use?
Michael:
Ventricular assist devices, which comprise a significant amount of our preclinical work in this technology, have historically been dominated by just a few technologies and manufacturers. Almost all of those companies are trying to increase the approved duration of use, develop safer and more effective circuits to and expand utilization.
New competition is entering the market via companies attempting to leverage new interventional technologies like improved pumps, controllers or catheters capable of performing the same functions of legacy heart and lung machines or bulkier surgically implanted devices. Commonly called percutaneous ventricular assist devices (pVADs) these newer technologies can be an excellent stop-gap alternative and minimize invasive surgeries to keep someone alive while they await surgery for a heart transplant or valve implantation.
Many approved ventricular or circulatory assist devices were originally developed, and approved for short-term management of six to twelve hours or slightly longer term of twenty four to forty eight hours. Most companies with approved devices on the market and in clinical use are seeking to get indications now for seven to fourteen days or even longer.
At the end of the day, these technologies are about buying time for the patient until a permanent solution can be achieved and maintaining healthy circulation in patients, which leads to better outcomes long term. This explains in large part why we are seeing manufacturers need the preclinical data required as they seek expanded indications for durations of use from days to weeks and test novel device components.
Paul: What’s the key unmet clinical need driving innovation?
Michael:
 First, these devices, like the patients whose lives depend upon them, need specialized care. That care is very commonly provided by ICU nurses who are with the patient and the machine every minute of the day. The device and the patient need constant monitoring. It’s not a sustainable long-term situation.
First, these devices, like the patients whose lives depend upon them, need specialized care. That care is very commonly provided by ICU nurses who are with the patient and the machine every minute of the day. The device and the patient need constant monitoring. It’s not a sustainable long-term situation.
The first goal is to make these devices perform their function with greater simplicity, less monitoring and management and reduction in coagulation. Having these devices perform with the relative simplicity of common EKG devices would represent a significant improvement in the provision of care for all concerned. Currently, these devices and the patients that rely on them require a team of three highly trained nurses working eight hour shifts or more managing just one or two patients each.
Second, these devices need highly specialized deployment. The inlet and outlet pump placement requires precision within centimeters or millimeters. It then must be secured to the skin to ensure it does not move when the patient does. (This is part of the issue that makes preclinical models important and limited). Making the deployment easier is a strong unmet clinical need for these devices.
It bears repeating, new circulatory or ventricular assist devices won’t meet the clinical demand as a one or two day solution. That often isn’t enough time for a transplant to be identified or heart valve to be made, shipped and surgery to be scheduled and performed. That process can easily be seven days or more.
Paul:
More specifically to preclinical work, what are you seeing?
Michael:
Manufacturers want to know how far we can go on approved devices. The FDA typically requires 2x the requested indication be conducted in preclinical models. This means that for a 7 day indication, animals will need to be on the devices for 14 days, stanchioned and under constant supervision and care. Due to these constraints, sheep or calves are almost always selected due to their docile nature, cardiovascular anatomy size and sufficient volume of blood flow.
Anticoagulation is a common challenge in preclinical work for these devices, both in the subject and in the machine. [Editor’s note: Dr. David Ku is working on a solution to connector technology with Georgia Tech Pediatric Technologies to reduce clotting in ECMO machines.]
Another factor is just the simple management of the devices, cables and tubing for preclinical work, as it is in the clinical setting, which we mentioned previously, and which very new technologies seek to address.
VAD and ECMO technologies are typically inserted in the patient via jugular, carotid or femoral arteries. In preclinical work, we are often restricted to the neck, chest (via thoracotomy) or back (via retroperitoneal access) because even in particularly docile subjects risk of kinking, separation or breaking if placed in femoral arteries or veins once the animal is recovered and standing. In devices with high blood volume and pump speed requirements, models are almost commonly limited to calves due to their larger hearts and volume of blood, another reason preclinical work in these technologies can quickly become quite expensive.
Paul:
We’ve talked in the past about pilot preclinical tests as high value learning opportunities in order to increase the likelihood of a successful, though ‘heavy’ and highly expensive GLP study. Have innovators and investors taken heed to this approach and been doing more of them?
 Michael:
Michael:
Yes, especially because there is less knowledge and increased risk with the impact of these much longer durations on the blood due to mechanical elements, which were only originally proven and approved for short timeframes. Hemolysis and thrombus formation are constant risks that need to be tested thoroughly. These VAD and ECMO survival models are a constantly challenging model to monitor, maintain and document these test animals for such long durations at a GLP compliant level. It’s an evolving field in preclinical models but one that is increasingly in demand.
Paul:
If someone is evaluating their new CAD technology’s readiness for preclinical work, what are the most important things to know?
Michael:
First, know the preclinical model and its implications. The difference in anatomy in sheep and calves versus humans means surgical deployment and placement in parts of the subject’s anatomy that would never be deployed in the same part of the anatomy as a human. And even percutaneous technologies may require surgical implantation for preclinical models, which is not how they may be intended to be used for use in humans.
Second, it is incredibly important, and a massive cost saving for development purposes, to have sufficient confidence in bench testing. Bench testing should approach new ‘design lock’ on pump function, for example, prior to any preclinical testing. Will the controller or motor even meet the running endpoint of seven to fourteen days on its own? If you rush into the study with prototype test articles and initiate the test, but a mechanical element like the controller or motor fails on day one and you planned to run for eight days it can create a wasteful scenario.
 Lastly, you must have confidence in, and possibly allow for learning among, your surgical team. Our internal teams have deployed dozens of these technologies, but due to either contracting or availability, innovators who bring in their own surgeons may not have the anatomic familiarity with the subject or model, which means pilot studies almost always need some changes to the planned deployment of the device to accommodate the preclinical model.
Lastly, you must have confidence in, and possibly allow for learning among, your surgical team. Our internal teams have deployed dozens of these technologies, but due to either contracting or availability, innovators who bring in their own surgeons may not have the anatomic familiarity with the subject or model, which means pilot studies almost always need some changes to the planned deployment of the device to accommodate the preclinical model.
At the end of the day, companies with preclinical needs for these technologies should probably plan for two to three pilot studies, which can make GLP studies which can easily reach six figures in cost, more efficient.
Get in touch
If you are evaluating your circulatory or ventricular assist technologies readiness for preclinical, or if you have an idea or technology earlier in its pathway that may need regulatory pathway evaluation, IP or freedom to operate assessment or other design and development concern, it’s never too early to get in touch.
Contact us via the form below today.
Related content: